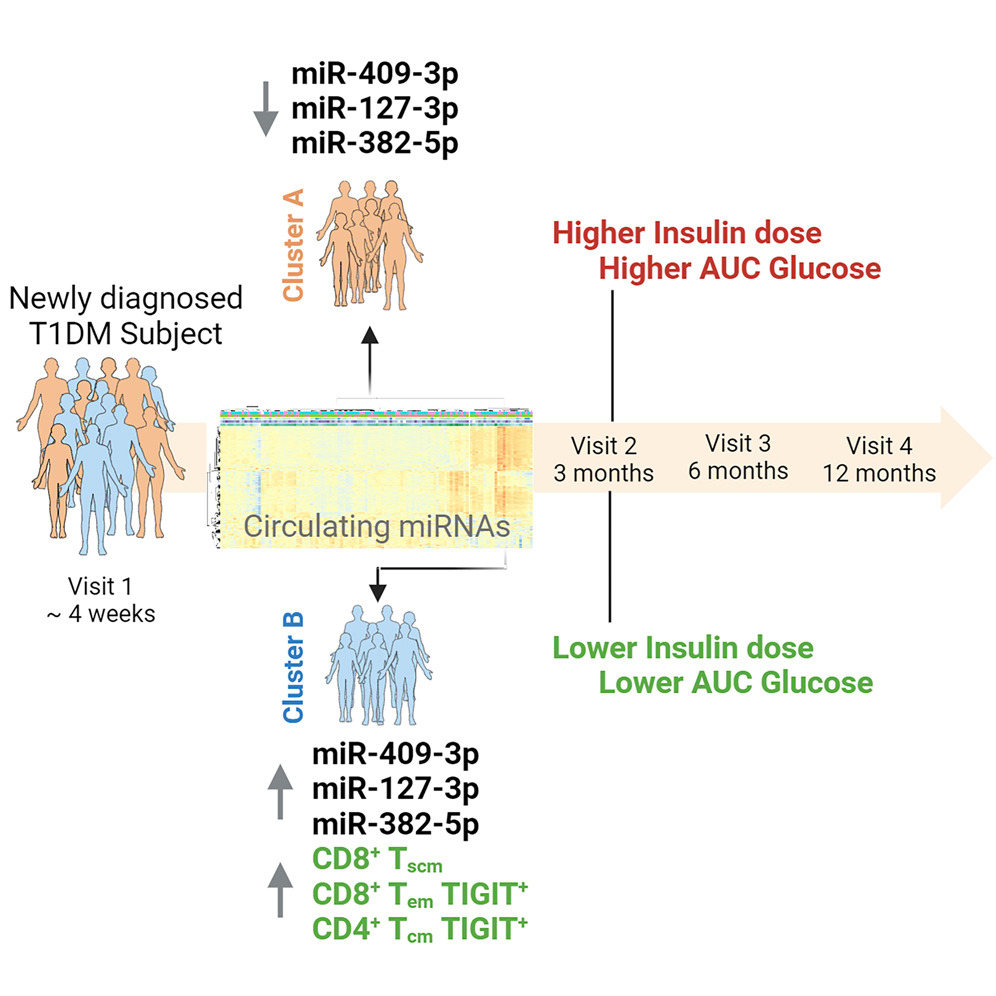
As the Head of the Department of Medicine, Surgery, and Neuroscience at the University of Siena, and Director of Diabetes and Clinical Nutrition Units at Policlinico University Hospital in Siena, Prof Dotta oversaw the international collaborative work. Beyond the National Center, additional support came from the European Union as part of the INNODIA project. Using advanced RNA sequencing technology that only requires a few microliters of blood, researchers identified a class of small noncoding RNAs, called circulating microRNAs, which could offer valuable diagnostic and prognostic tools for T1DM.
Latest news

National Center Patronage Puts Precision Medicine at the Heart of Microfluidic Horizons 2026

Extended Application Deadline – Legal Officer

Naples Hosts Global Dialogue on RNA Therapeutics as Italy’s National Center Takes Center Stage

INSPIRE Morning Talk Explores Impact and Future of Italy’s PNRR Research Initiatives

Advanced Cell and Gene Therapy Workshops 2026